Table of Contents
Introduction
Last year, the Air Quality Index (AQI) in New Delhi crossed 800+ for PM2.5, one of the worst levels recorded. And it wasn’t just Delhi, nearby areas were affected in the same way.
During that time, one common symptom was seen everywhere and that was persistent cough
Now, any curious person would ask, “Why is this happening?”
The answer is simple. This cough is actually your body’s response to polluted air entering your airways.
It’s your immune system trying to protect your lungs from harmful particles.
For most people, this was temporary. As the air quality improved, the symptoms went away. But unfortunately, for some people, it doesn’t go away. For them, this irritation becomes chronic (long-term) and slowly develops into a serious lung condition.
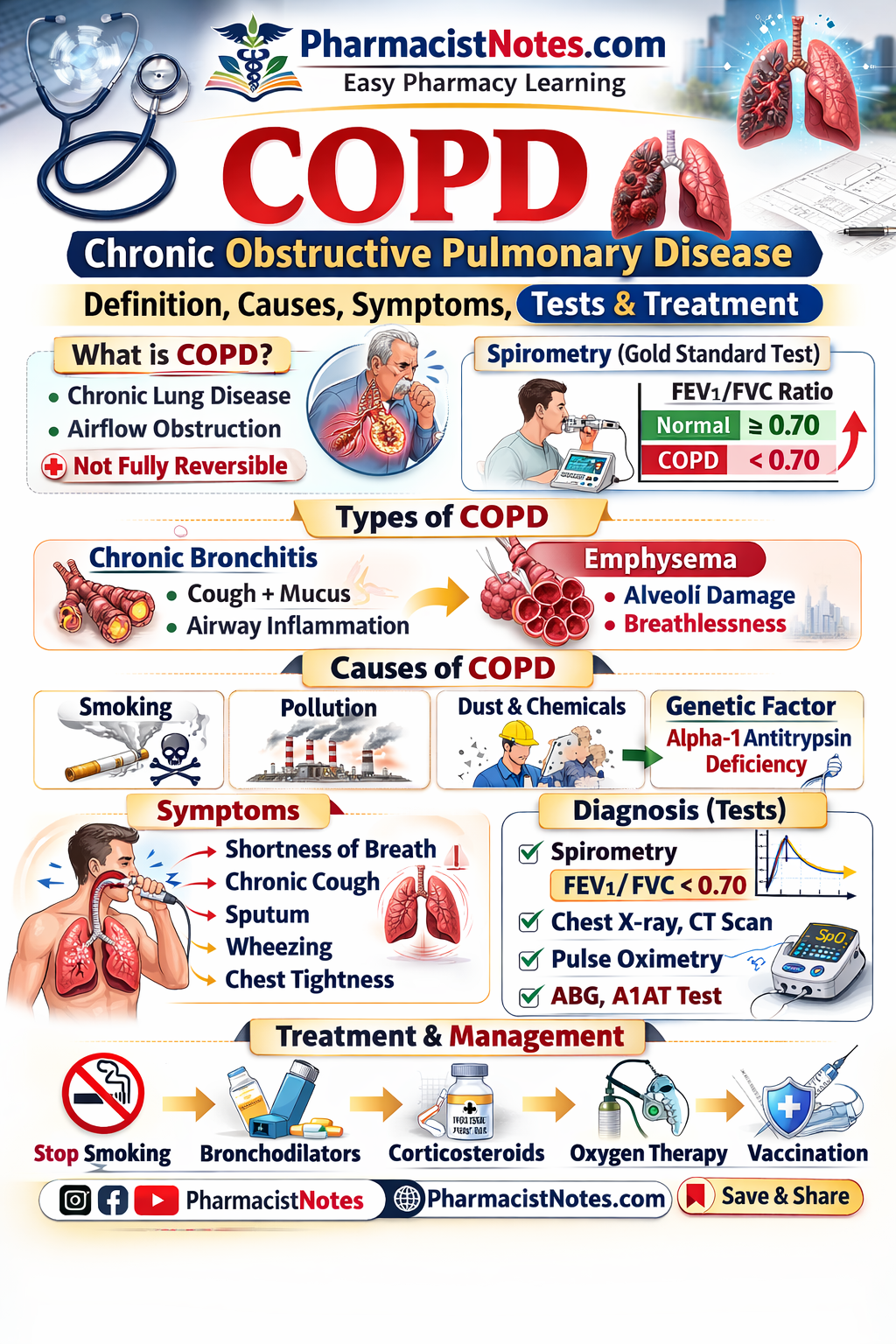
Today, we’re going to understand this chronic disease, often linked with polluted air: COPD (Chronic Obstructive Pulmonary Disease)
Bad air is not the only cause of COPD, but in countries like India, it is definitely one of the major contributing factors.
It is a long-term lung disease in which airflow is blocked and breathing becomes difficult.
In this disease, the airways become narrow and the lungs get damaged, so the patient cannot breathe properly.
COPD mainly includes two conditions:
- Chronic bronchitis – airways become inflamed and produce excess mucus, causing chronic cough and breathing difficulty.
- Emphysema – alveoli (air sacs) are damaged and destroyed, reducing oxygen exchange and causing breathlessness.
What is COPD?
COPD (Chronic Obstructive Pulmonary Disease) is a long-term lung condition in which the airways become narrow, making it difficult to breathe.
In layman terms, it’s a disease where air cannot flow in and out of the lungs properly.
Over time, the lungs get damaged, and breathing becomes more difficult — especially during activities like walking, climbing stairs, or even talking.
Unfortunately, COPD is not fully reversible, because the damage to the lungs is permanent. However, with proper treatment and care, its progression can be slowed down.
COPD doesn’t happen suddenly.
It develops slowly over time due to repeated exposure to harmful particles and gases.
Let’s understand the main causes:
1. Smoking (Most Common Cause)
Smoking is the leading cause of this disease worldwide.
This includes:
- Cigarettes
- Bidi
- Passive smoking (breathing smoke from others)
When a person smokes regularly:
- The lungs get damaged
- Airways become inflamed
- Breathing gradually becomes difficult
Over time, this damage becomes permanent.
2. Air Pollution (Major Cause in India)
In countries like India, air pollution plays a huge role.
Common sources include:
- Vehicle smoke
- Industrial pollution
- Biomass fuel (wood, chulha smoke)
Continuous exposure to polluted air irritates the lungs and slowly leads to chronic damage.
3. Occupational Exposure
People working in dusty or polluted environments are at higher risk.
For example:
- Factory workers
- Miners
- Construction workers
Long-term exposure to dust and chemicals can damage the airways and lungs.
4. Genetic Factor (Rare)
In some cases, It can develop due to a genetic condition called: Alpha-1 Antitrypsin Deficiency
Alpha-1 antitrypsin is a protein that protects lungs.
If this protein is low:
- Lungs get damaged
- COPD develops
Pathophysiology (What happens in lungs)
Before we understand the physiology, let’s first see what happens in normal lungs and then compare it with what changes in COPD.
| Healthy Lungs | COPD Lungs | |
|---|---|---|
| Airways | Open and clear | Narrow and inflamed |
| Airflow | Air moves easily in and out | Airflow becomes restricted |
| Mucus | Normal amount | Excess mucus blocks airways |
| Alveoli (Air sacs) | Intact and elastic | Damaged and lose elasticity |
| Breathing | Easy and effortless | Difficult and laboredIn a healthy person, the airways are open and clear, so air can move in and out of the lungs without any difficulty. The air sacs (alveoli) are also intact and elastic, which helps in proper exchange of oxygen and carbon dioxide. Because of this, breathing feels normal and effortless, even during physical activity. In this disease, this normal structure is gradually damaged. The airways become narrow and inflamed, and excess mucus starts blocking them. At the same time, the alveoli lose their elasticity and get damaged, which reduces the efficiency of oxygen exchange. As a result, air gets trapped inside the lungs, and the person starts experiencing shortness of breath and difficulty in breathing, even during simple daily activities. |
In a healthy person, the airways are open and clear, so air can move in and out of the lungs without any difficulty. The air sacs (alveoli) are also intact and elastic, which helps in proper exchange of oxygen and carbon dioxide. Because of this, breathing feels normal and effortless, even during physical activity.
In this disease, this normal structure is gradually damaged. The airways become narrow and inflamed, and excess mucus starts blocking them. At the same time, the alveoli lose their elasticity and get damaged, which reduces the efficiency of oxygen exchange. As a result, air gets trapped inside the lungs, and the person starts experiencing shortness of breath and difficulty in breathing, even during simple daily activities.
Symptoms of COPD
Main symptoms:
In day to day OPD we see patients with following symptoms,
- Patients complaining shortness of breath (make sure it is not a heart problem)
- Patients saying he has chronic cough, persistent cough
- Patients confirming sputum production
- Wheezing sound while breathing
- Complaint of chest tightness (carefully ask patient and differ from angina)
It is also important to understand that most patients with this disease are elderly.
Symptoms like shortness of breath and chest tightness can sometimes look very similar to conditions like angina or even a heart attack.
In practice, once we identify one problem, we often tend to rule out other possibilities — this is quite natural.
But we should always remember that both conditions can exist at the same time.
As a pharmacist, it is important to stay alert.
If a patient presents with such symptoms, we should always advise them to seek medical attention immediately, especially if there is any doubt.
And if you are working in a hospital setting and feel that something might have been missed,
it is absolutely appropriate to communicate this with the doctor.
There is no harm in speaking up. It can actually make a significant difference in patient care.
Severe symptoms:
- Fatigue
- Weight loss
Severe symptoms occur as there is lack of oxygen in the body. If you see a patient with these symptoms, advise them to visit hospital.
Is COPD reversible?
Unfortunately it is not fully reversible.
But treatment can:
- Improve symptoms
- Slow disease progression
It is not fully reversible because the lung tissue and airways are permanently damaged.
- The alveoli (air sacs) are destroyed
- The airway walls become thick and narrow
- Elasticity of lungs is lost
These structural changes cannot return to normal.
Diagnostic Tests for COPD
1. Spirometry (Gold standard test)
Spirometry is the most important and widely used test for diagnosing it.
It gives a clear picture of:
- Whether the disease is present or not
- How severe the airflow obstruction is
This test measures how much air a person can inhale and exhale, and how quickly they can breathe out.

It measures lung function.
Key result:
FEV1/FVC ratio < 0.70 confirms it.
FEV₁ is the volume of air exhaled in the first second, and FVC is the total volume of air exhaled forcefully after full inspiration.
FEV₁/FVC ratio less than 0.70 indicates airflow obstruction and confirms it.
2. Chest X-ray
Shows lung damage and hyperinflation.
3. CT scan
Shows detailed lung damage.
Useful for detecting emphysema.
4. Pulse oximetry
Measures oxygen level in blood.
Low oxygen indicates severity.
5. ABG test (Arterial Blood Gas)
Measures oxygen and carbon dioxide levels.
Used in severe condition.
6. Alpha-1 Antitrypsin test
Used to detect if this disease is genetic or not.
Treatment of COPD
1. Bronchodilators (First-line drugs)
These drugs relax airway muscles.
Examples:
- Salbutamol
- Ipratropium
- Tiotropium
- Theophylline
2. Corticosteroids
Reduce inflammation.
Example:
- Budesonide
3. Oxygen therapy
Used in severe conditions. I have seen patients rushing to emergency during oct – dec months in north india
4. Lifestyle changes
Important lifestyle tips:
- Stop smoking
- Avoid pollution
- Regular exercise
- Healthy diet
Summary
Chronic Obstructive Pulmonary Disease is a chronic, progressive lung disease characterized by persistent airflow obstruction and breathing difficulty. It mainly includes chronic bronchitis, which causes airway inflammation and excess mucus production, and emphysema, which involves destruction of alveoli and reduced gas exchange. The most common cause of it is long-term smoking, but air pollution, occupational exposure to dust and chemicals, and genetic factors such as alpha-1 antitrypsin deficiency can also contribute.
In COPD, the airways become narrowed and lung tissue is permanently damaged, leading to symptoms such as shortness of breath, chronic cough, sputum production, and wheezing. Unlike asthma, It is not fully reversible because the structural damage to the lungs and airways is permanent. Spirometry is the gold standard diagnostic test, and a reduced FEV₁/FVC ratio (< 0.70) confirms airflow obstruction.
Treatment of COPD focuses on relieving symptoms, improving airflow, and slowing disease progression. Bronchodilators such as salbutamol, ipratropium, and tiotropium are first-line drugs, while corticosteroids and oxygen therapy are used in more severe cases. Smoking cessation, avoiding pollution, regular exercise, and proper medical management are essential to improve quality of life and prevent further lung damage.
| Feature | Description |
|---|---|
| Full form | Chronic Obstructive Pulmonary Disease |
| Definition | COPD is a chronic, progressive lung disease characterized by persistent airflow obstruction and breathing difficulty. |
| Nature of disease | Chronic and progressive |
| Reversibility | Not fully reversible due to permanent lung damage |
| Main components | Chronic bronchitis and emphysema |
| Chronic bronchitis | Airway inflammation and excess mucus production causing airway narrowing |
| Emphysema | Destruction of alveoli leading to reduced gas exchange |
| Main cause | Smoking (most important cause) |
| Other causes | Air pollution, occupational exposure, biomass fuel smoke |
| Genetic factor | Alpha-1 antitrypsin deficiency |
| Main symptoms | Shortness of breath, chronic cough, sputum production, wheezing |
| Pathophysiology | Airway inflammation, mucus |
FAQs
1. What is COPD?
COPD is a chronic lung disease that causes airflow obstruction and breathing difficulty due to airway narrowing and lung damage.
2. What is the main cause of COPD?
The main cause of COPD is long-term smoking. Other causes include air pollution, occupational dust exposure, and genetic factors.
3. Is COPD reversible?
No, It is not fully reversible because it causes permanent structural damage to the lungs and airways. However, treatment can improve symptoms and slow disease progression.
4. What are the main symptoms of COPD?
Common symptoms include shortness of breath, chronic cough, sputum production, wheezing, and chest tightness.
5. What is the gold standard test for COPD?
Spirometry is the gold standard test. A FEV₁/FVC ratio less than 0.70 confirms COPD.
6. What are the main drugs used in COPD?
The main drugs used in COPD are bronchodilators such as salbutamol, ipratropium, and tiotropium. Corticosteroids and oxygen therapy are used in severe cases.
7. What is the genetic cause of COPD?
Alpha-1 antitrypsin deficiency is the main genetic cause of COPD. It leads to lung tissue damage even in non-smokers.
8. What is the difference between COPD and asthma?
COPD is usually irreversible and caused by smoking, while asthma is reversible and mainly caused by allergies.
9. Can COPD be prevented?
Yes, It can be prevented by avoiding smoking, reducing exposure to air pollution, and using protective equipment in dusty environments.
10. Who is at high risk?
People who smoke, are exposed to air pollution, work in dusty environments, or have genetic predisposition are at higher risk.


3 thoughts on “Life-Changing Insights on COPD: Symptoms, Causes, Diagnosis & Treatment Explained”